It’s not a full collapse. Not a rock bottom.
But something’s different—and deep down, you know it.
You’ve been here before, which is why this feeling is harder to ignore.
If you’ve found yourself quietly wondering whether it’s time to step back into more support, even something like structured daytime care, this might be the moment worth listening to.
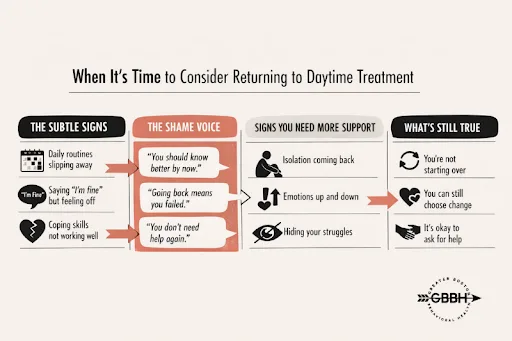
It Doesn’t Start Loud—It Starts Subtle
Most people don’t wake up one day and think, “I need help again.”
It’s quieter than that.
You skip a routine that used to keep you grounded.
You start telling yourself, “I’ve got this,” but feel less steady saying it.
The things that once worked… don’t hit the same.
It’s not failure. It’s drift.
And drift is how people slowly lose their footing without realizing it.
The Voice in Your Head Might Be Lying to You
There’s a specific kind of shame that shows up after time away from treatment.
It says things like:
- “You should know better by now.”
- “You already had your chance.”
- “Going back means you failed.”
But that voice isn’t wisdom. It’s fear.
Coming back doesn’t erase your progress.
It proves you’re paying attention.
You’re Not Back at the Beginning—Even If It Feels That Way
This part matters more than most people realize.
You’re not starting over.
You’re returning with insight.
You know your patterns better now.
You recognize the warning signs faster.
You’ve already built pieces of a life that felt more stable.
That doesn’t disappear because things got shaky.
It means you’re in a different position this time—one with more awareness, not less.
🚩 Signs You Might Need More Support Right Now
You don’t need everything to fall apart to justify stepping back in.
Sometimes it looks like:
- You’re more emotionally reactive than usual
- Isolation is creeping back in, even if you’re still “functioning”
- Your coping tools feel harder to access or less effective
- You’re minimizing things you wouldn’t have ignored before
- Part of you is hoping no one notices
If even one of those hit, it’s worth paying attention.
Why a Higher Level of Care Can Feel Different the Second Time
The first time, everything is new. Uncertain. Sometimes overwhelming.
The second time? It’s more honest.
You’re not there because someone told you to go.
You’re there because you felt something slipping—and chose to respond.
That shift matters.
Many people find that returning to a Partial Hospitalization Program at this stage feels less like starting over and more like reinforcing what they already built.
Like tightening bolts before something breaks.
You’re Allowed to Catch It Early
There’s a quiet strength in not waiting until things get worse.
You don’t have to earn help through suffering.
You don’t have to prove it’s “bad enough.”
Sometimes the bravest move is saying:
“I see where this could go—and I don’t want to go there again.”
That’s not weakness. That’s awareness in action.
The Door Is Still Open And It Always Will Be
If you’re reading this, you haven’t lost everything.
You’re noticing. You’re thinking. You’re questioning.
That means something in you is still very much intact.
And that part of you?
It’s worth protecting.
If something feels like it’s slipping, you don’t have to wait for it to fall.
Call (888) 450-3097 or explore your options for treatment in Boston to learn more about how we can support you in finding your footing again.