You don’t have to hit a breaking point to deserve support.
A lot of people wait anyway.
If you’ve been quietly wondering whether it’s time to do something more structured—something consistent—this is for you. You can explore your next step, like this structured daytime care option, without everything falling apart first.
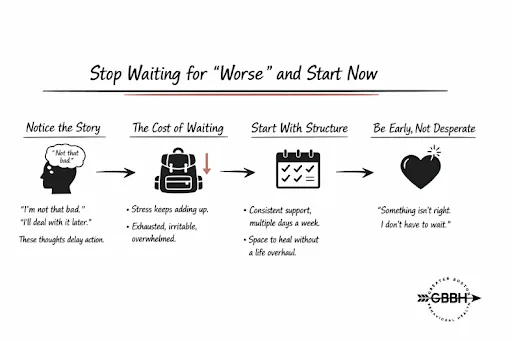
Notice the Story You Keep Telling Yourself
“I’m not that bad.”
“I can still function.”
“I’ll deal with it later.”
These thoughts sound reasonable. They’re also the most common way people delay getting help.
From a clinical perspective, the earlier someone steps into consistent support, the easier it is to stabilize. Not because they’re “worse”—but because they’re catching it before exhaustion becomes collapse.
Pay Attention to the Cost of Waiting
The impact isn’t always dramatic. It’s subtle.
- You’re more irritable than you used to be
- Small things feel overwhelming
- Rest doesn’t actually recharge you
- You keep pushing through, but it’s getting heavier
Waiting doesn’t keep things neutral. It slowly raises the baseline of stress.
Think of it like carrying a backpack that keeps getting heavier one pound at a time. You adjust… until one day you can’t.
Get Honest About What “Functioning” Really Means
A lot of people I work with are technically functioning.
They’re working. Showing up. Responding to texts. Smiling when needed.
But inside, they’re stretched thin.
Functioning isn’t the same as feeling okay.
And it’s not a requirement to be falling apart before you deserve more support.
Start With Structure, Not a Huge Life Change
You don’t need to flip your entire life upside down.
A better place to start is adding structure.
Consistent daytime support—multiple days a week—creates space to actually process what’s going on instead of just managing symptoms between responsibilities.
This isn’t about stepping away from your life.
It’s about finally having support inside of it.
Let Yourself Be Early Instead of Late
There’s a quiet kind of courage in starting before things get worse.
Most people don’t talk about that part.
They talk about rock bottom. Crisis. Last chances.
But some of the strongest decisions happen earlier—when something inside you says,
“Something isn’t right, and I don’t want to wait until it gets worse.”
That voice matters.
You Don’t Have to Be Sure—Just Willing
You don’t need certainty to begin.
You don’t need a label.
You don’t need a dramatic story.
You just need a small willingness to explore something different.
That’s enough to start.
What Taking the First Step Can Look Like
You don’t have to commit to everything today.
You can:
- Ask questions
- Learn what your options actually look like
- See if the schedule and support fit your life
- Talk to someone who understands what you’re navigating
That’s it. No pressure—just movement.
You’re allowed to take this seriously before it becomes unbearable.
You’re allowed to choose support before you’re desperate for it.
If something in this resonated, trust that.
Call (888) 450-3097 or explore your options for treatment in Boston to learn more about our Partial Hospitalization Program services in your area.